GORE® VIABAHN® Device family
Disease Overview
Join the next generation of care in the treatment of aortoiliac occlusive disease
Aortoiliac occlusive disease (AIOD) – An increasingly complex condition
The incidence of AIOD is increasing,1 leaving more patients vulnerable to a disease that, untreated, can cause pain, tissue loss and amputation.
- Roughly 10% of U.S. adults (over 60 years old) are affected by peripheral arterial disease (PAD).1,2
- Roughly 33% of PAD cases involve the iliac arteries.3
Guidelines for treating AIOD
TASC II A AND B LESIONS:
Guidelines recommend an endovascular approach.4
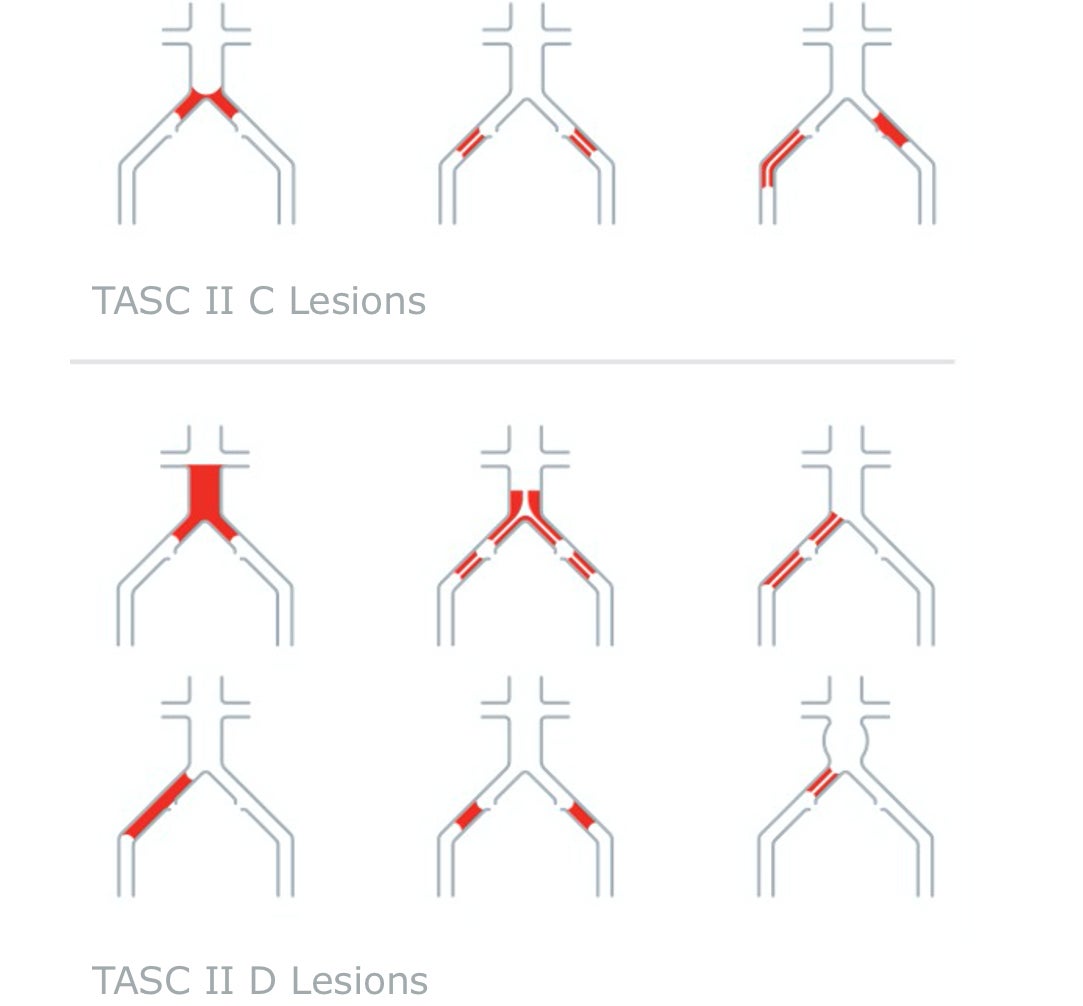
TASC II C AND D LESIONS:
Guidelines recommend surgery, although multiple consensus and practice guidelines now generally endorse an endovascular-first strategy in experienced endovascular centers.4-7
Potential obstacles of endovascular treatment
CHALLENGES:
- Tortuous anatomies
- Severe stenosis
- Highly calcified occlusions
RISKS:
- Perforation or rupture of the iliac arteries and aortic bifurcation occurs in nearly 4% of cases and can be a life-threatening complication.8-11
- Rupture can be difficult to identify on the final angiogram, and may occur postoperatively, causing acute bleeding and hypotension.12, 13
* As used by Gore, Heparin Bioactive Surface refers to Gore’s proprietary CBAS Heparin Surface.
- Criqui MH, Aboyans V. Epidemiology of peripheral artery disease. Circulation Research 2015;116(9):1509-1526.
- Cooke JP, Chen Z. A compendium on peripheral arterial disease. Circulation Research 2015;116(9):1505-1508.
- Kumar V. Defining the role of covered stents in aorto-iliac interventions. Interventional Cardiology 2013;5(1):45-52.
- Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, Fowkes FG; TASC II Working Group. Inter-Society consensus for the management of peripheral arterial disease (TASC II). Journal of Vascular Surgery 2007;45(1)Supplement S:S5-S67.
- Klein AJ, Feldman DN, Aronow HD, et al; Peripheral Vascular Disease Committee for the Society for Cardiovascular Angiography and Interventions. SCAI expert consensus statement for aorto-iliac arterial intervention appropriate use. Catheterization & Cardiovascular Interventions 2014;84(4):520-528.
- Rossi M, Iezzi R. Cardiovascular and Interventional Radiological Society of Europe guidelines on endovascular treatment in aortoiliac arterial disease. Cardiovascular & Interventional Radiology 2014;37(1):13-25.
- European Stroke Organisation, Tendera M, et al; ESC Committee for Practice Guidelines. ESC Guidelines on the diagnosis and treatment of peripheral artery diseases: document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extremity arteries: the Task Force on the Diagnosis and Treatment of Peripheral Artery Diseases of the European Society of Cardiology (ESC). European Heart Journal 2011;32(22):2851-2906.
- Jongkind V, Akkersdijk GJ, Yeung KK, Wisselink W. A systematic review of endovascular treatment of extensive aortoiliac occlusive disease. Journal of Vascular Surgery 2010;52(5):1376-1383.
- Indes JE, Pfaff MJ, Farrokhyar F, et al. Clinical outcomes of 5358 patients undergoing direct open bypass or endovascular treatment for aortoiliac occlusive disease: a systematic review and meta-analysis. Journal of Endovascular Therapy 2013;20(4):443-455.
- Piazza M, Squizzato F, Dall'Antonia A, et al. Outcomes of self expanding PTFE covered stent versus bare metal stent for chronic iliac artery occlusion in matched cohorts using propensity score modelling. European Journal of Vascular & Endovascular Surgery 2017;54(2):177-185.
- Squizzato F, Piazza M, Pulli R, et al; ILIACS Registry Group. Covered versus bare metal kissing stents for reconstruction of the aortic bifurcation in the ILIACS registry. Journal of Vascular Surgery. In press.
- Sobrinho G, Albino JP. Delayed rupture of the external iliac artery after balloon angioplasty and stent placement. Journal of Vascular & Interventional Radiology 2008;19(3):460-462.
- Allaire E, Melliere D, Poussier B, Kobeiter H, Desgranges P, Becquemin JP. Iliac artery rupture during balloon dilatation: what treatment? Annals of Vascular Surgery 2003;17(3):306-314.